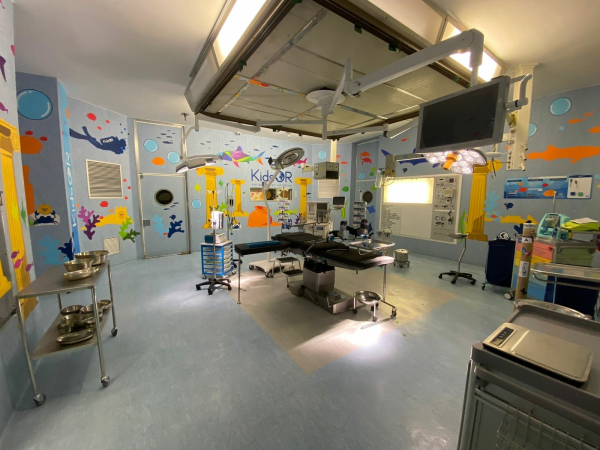
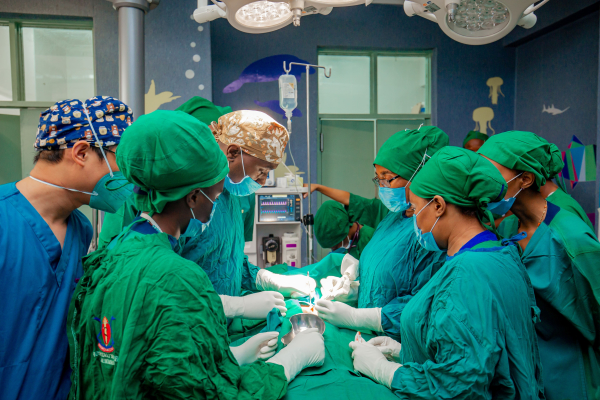
Q&A with trainee paediatric surgeon Dr Tumusiime
Dr Tumusiime, who graduated from medical school in 2016, is currently undertaking a paediatric surgery traineeship at Kenyatta National Hospital (KNH) in Nairobi, Kenya, thanks to the surgical training scholarships provided by our partnership with Smile Train.
Allan recently relocated to Kenya after working as a general surgeon at St Mary’s Lacor Hospital and Mulago hospital in Uganda. We spoke to him about his journey.
How did you end up at Kenyatta National Hospital?
While still in Mulago, I was interested in a certain classified case that was happening at KNH. I asked my supervisors if I could go - and likewise reached out to the staff at KNH who approved my visit. As paediatric surgeons, we are not many in the region and we share key information happening around. That is how I came to know of this case.
While at Kenyatta Hospital, I looked at the wards… interacted frequently with the bosses... I felt there were more cases, more paediatric surgical residents than where I was based in Mulago. Further, at KNH, because most of the patients are covered by the Kenyan government medical system (National Hospital Insurance Fund-NHIF) a paediatric surgeon can administer more treatment options (do more investigations on a patient where need be). Back at home people pay from their pocket and you can only prescribe treatment which they can afford.
Another thing is the everyday interaction with different paediatric surgeons. This helps a lot in knowledge acquisition. KNH alone has about 16 surgeons that’s double the number of paediatric surgeons in the whole of Uganda.
The one case I’m happy to be carrying out is….
It is a simple procedure but has profound implication. Basically, all babies at eight weeks, their intestines come out to give the liver a chance to grow. They go back at 12 weeks but for some babies they don’t, hence they are born with them outside. Usually, we would return the intestines bits by bits, a routine that would take one to 12 weeks in total. In this process, children get infections/ sick a lot. This, however, has changed overtime whereby we are putting all the intestines back and placing the umbilicus on top. There are less infections, they recover quicker and spend only about a week in the ward. Gastroschisis is one of the most common paediatric surgeries requested, as every month about a dozen kids need treatment for it.
What I love about the training...
The training at Kenyatta National Hospital is a lot more engaging, and I love that the consultants are a lot more available to teach. A paediatric surgeon is always physically present for every major elective case. Three times a week, consultants lead the ward rounds. Once a week, two consultants are physically present in the paediatric surgery clinic. The more contact hours with consultants, the merrier!

Dr Tumusiime with Africa Director Rosemary Mugwe
I've always found it easy to be a children's doctor. The hours are long, and the work is gruelling, but children are magnetic - I'm always drawn to them.
What do you find challenging?
I've always found it easy to be a children's doctor. The hours are long, and the work is gruelling, but children are magnetic - I'm always drawn to them, even when at the limits of physical exhaustion.
As a first year fellow, I am the first on call. This implies that I am the first contact the children will have in paediatric surgery, and a lot of my work will be clerical and procedural. As such, the workload can be quite sizable. The call lasts a week, and on most days, one may get three or four hours of sleep every day. It is hard in the beginning, but the human body is incredibly resilient, and it eventually adapts.
What has been the standout moment in the last three month of your studies?
There have been many but, I'd go with our first sutureless (stitchless) closure of gastroschisis at KNH. The obstetricians were able to diagnose gastroschisis intrauterine (this is the case I earlier talked about of intestines being out of the tummy) with an ultrasound - something that rarely happens because most of our mothers have no prenatal ultrasounds. We were called to be part of the caesarean section and soon after the baby was delivered, I held her in my arms and carried her to a separate sterile table, and together with a fellow resident, Dr. Rossana Chevalavela, we were able to reduce all the bowel primarily and cover with the umbilical.
The child has since had a seamless recovery. We aim to make sutureless closure of gastroschisis the order of the day.
Are there more cases you’d like to share with us?
Generally, I have been involved in over 49 operations in the last three months, 25 of which I have done unsupervised. Besides the gastroschisis surgery, another key case I found transformative was my first posterior sagittal anorectoplasty on an 8 months old baby girl, under the guidance of Dr. Kayima Peter. It’s a complicated case. You are creating new muscles of/for the anus because the child was born without one.
This is a major case, and first year fellows anywhere would struggle taking one on, but I've worked with Dr. Kayima for over four years, and he felt that I could start on one - my incessant pleading not withstanding!
As one would expect, when we got to the business end of the procedure, the consultant became more and more involved, but overall, it was my case - I was primary. The operation went smoothly, and the postoperative period was just as smooth. We started dilation (opening) of the neoanus and we are confident that by school-age, she'll have a reasonably normal life.Q&A
Share article
Recent Posts



Similar Posts
Namibia prioritising the lives of children.
Paediatric surgery included in Namibia's healthcare strategy going forward