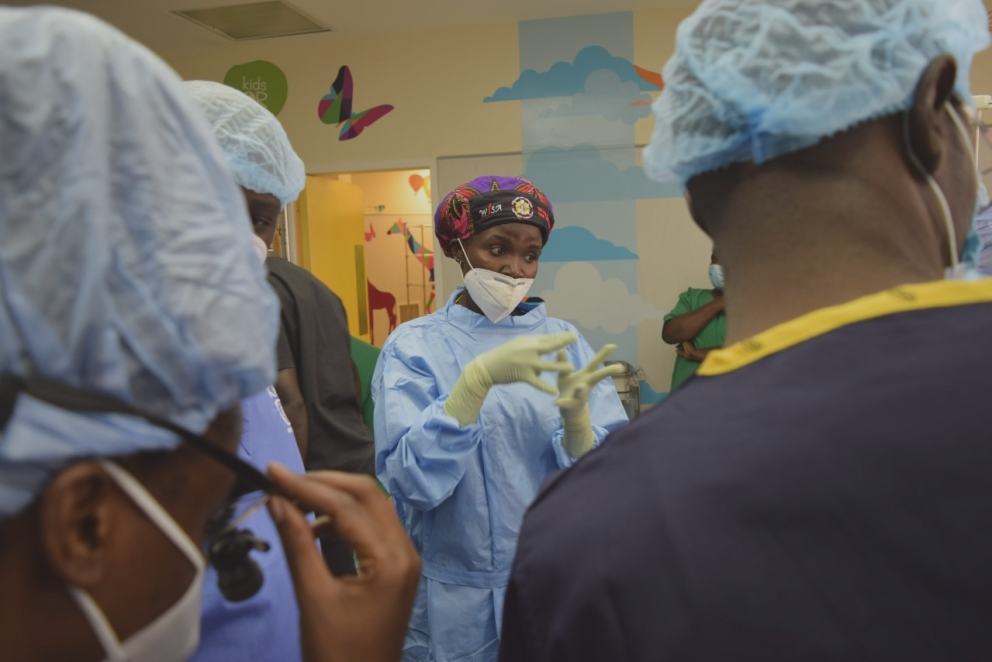
Putting the right tools in the right hands.
For a child requiring surgery, visiting Mulago Hospital in Uganda did not hold any guarantee of success. A lack of dedicated paediatric space and equipment meant that the sparce resources available to the local surgical team were concentrated on emergency cases, often resulting in children with non-urgent ailments being left to suffer on never-ending waiting lists.
Thankfully, this changed when KidsOR installed three brand new paediatric Operating Rooms at the hospital at the end of 2019.
For Dr. Phyllis Kisa, a paediatric surgeon in Mulago, the improvement this made to the hospital was huge.
“Having the Operating Rooms has made an enormous difference. We have access to these facilities at all times and are now performing more operations. We can take on more complex cases and are even conducting surgical camps without inconveniencing other users of the operating space like in the past.”
Dr. Kisa
As well as just having a dedicated space to operate, Dr. Kisa says the staff and patients in the hospital are benefiting from having the correct equipment for children’s surgery.
“Many times, we had to wait till a visiting surgeon came with their own tools for a surgery to be done. Some children on waiting lists were forced into waiting for their operation until they were older since we only had adult tools, but many died from complications arising from their conditions before surgery.”
Despite now having the right resources to hand, life as a paediatric surgeon in a low-and-middle- income country still contains its challenges.
“Every day we wake up, we deal with complex problems in children, making decisions that will impact them for life. This is not easy. The greater demand for paediatric anaesthesia services, which have not grown at the same rate as surgical services, can be quite crippling. We need buy-in from our own governments to advance care particularly in areas like surgery that are thought to be expensive and do not have the same visibility and advocacy like infectious conditions.”
And whilst Phyllis’ daily work is incredibly challenging, a lack of understanding surrounding surgical care from her government regarding funding makes life even more difficult.
“Most funding for children is in HIV, malaria, tuberculosis and little for correctable structural problems. My area is in correcting structural problems but there is little funding that is open to someone like me. Surgical services remain poorly understood and many look at the costs versus the cost benefit of correcting a surgical problem, while comparatively, you could spend a lot more treating the multitude of infectious conditions.”

Despite this, Phyllis is optimistic that the improvements made in Mulago will improve the services provided to the children of the area.
"For the first time, we have an operating room dedicated to paediatric specialties. Many of these departments had a huge waiting list of children, with benign problems that are not considered urgent, who were always bumped off their operating lists. This spreads out the workload making it easier for patients to access services.”
Help us supply tools to surgeons like Dr. Kisa

 Muhimbili National Hospital, 210222.png)
