Why are we letting so many children die?
Global health has traditionally focused on infectious disease control, mainly the big three – HIV, TB and malaria. Yet, despite almost a third of the global burden of disease requiring surgery as part of its treatment pathway, surgical services remain out of reach for most of the world’s children.
At the start of 2022 we estimate that 1.75 billion children don’t have timely, affordable access to surgical care.
Worse still, the funding models for global health remain rooted in the past. Donors, whether they be government or major INGO, seem to be wilfully ignoring the growing evidence of a shift in the causes of severe illness towards non-communicable diseases and injuries worldwide. Surgical conditions, ranging from trauma to appendicitis, now kill more people annually than HIV, TB and malaria combined – yet donors continue to drive their unchanging agendas.
I’m not saying that these programs were a mistake. Childhood mortality has decreased by 61% since 1990. Instead, the problem is a failure by the people running these programs to think about ‘what then?’. If you provide a vaccine to save a child from polio only to let them die from appendicitis, have you really made the world a better place?
And of course, you can argue that any one organisation ‘can’t do everything’. Fair enough, but when you’re responsible for spending hundreds of millions, even billions of dollars each year, that’s just not good enough.
The focus of donors on disease-specific programs does allow data to be captured and metrics to be measured. However, it has allowed them to hail great successes while leaving the majority of the world’s children without access to basic surgical services.
So, while these great successes in global health have been trumpeted, health systems have been ignored at a local level. Instead of building independent health services to achieve Universal Health Care (not coverage, care) the funding models of global health have chosen to see diseases instead of seeing people. They have flown in vaccination projects and then they’ve flown out. Local doctors and nurses haven’t been trained to anywhere near the number needed and children are suffering as a result.
54 million additional children’s surgical procedures are still needed every year around the world. This staggering total shines a very bright light on the failures of mission-based care to do anything other than perpetuate dependency – something the pandemic travel bans only served to highlight.
Yet there is hope…
Developing surgical services in a hospital involves strengthening many aspects of care. From diagnosis to recovery, the infrastructure needed and the team who grow around surgery improve care across the hospital.
Furthermore, surgical care does not need to be present in every village or community. It is an essential element of the health system that can be strengthened through local providers and can quickly roll out from National Referral Hospitals to District Hospitals in an extremely cost-effective way.
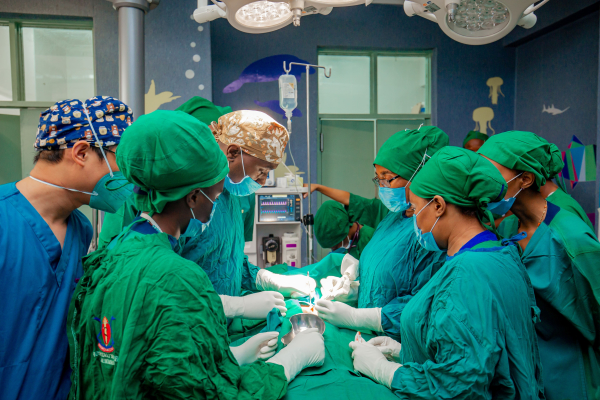
Even for the world’s most vulnerable and hard-to-reach children, like those in the Kakuma Refugee Camp in northern Kenya, surgical services can be developed and locally delivered with the right investment in people and infrastructure. If these children can receive the care they need from a local surgical team, then every child should be able to.
The challenge to achieve that goal is not insignificant. There is currently 1 paediatric surgeon for every 3 million children across LMICs. Achieving the Sustainable Development Goals by 2030 seems impossible when faced with such a huge shortage. But, again, there are training programs in place and no shortage of desire from local doctors to provide this care for their own nation’s children.
The question then can only be ‘why isn’t this happening?’
Perhaps it’s because donors haven’t shifted to follow the evidence around the epidemiology of disease; or because there is still no recognition that health is a global activity in which we are all involved? Maybe there’s just no recognition that the voices, needs and demands of people in low-resource settings need to be listened to; or perhaps it’s simply a failure to realise that the national interests of high-income countries are best served by strengthening the health systems of low- and middle-income countries.
In reality, I suspect it’s a mixture of all four plus a good dose of not wanting to move beyond missions (and I’m sure a hundred other reasons). However, the simple truth is there are children dying from diseases we know how to treat.
We are choosing not to support the local system to care for these children, the big donors are choosing to ignore even the WHO’s building blocks framework for investing in health development and nations are forced to remain in dependency as a result.
And I, for one, think that’s unforgivable…
End.
Garreth Wood is Co-founder and chairman of Kids Operating Room
Share article
Recent Posts



Similar Posts
Namibia prioritising the lives of children.
Paediatric surgery included in Namibia's healthcare strategy going forward